Empower Your Journey: The Vital Connection Between HSG Procedure and IVF
In the realm of fertility treatments, the HSG (hysterosalpingogram) procedure stands out as a crucial diagnostic tool that can significantly impact the success of in vitro fertilization (IVF). This comprehensive guide explores the pivotal role of the HSG procedure in IVF, shedding light on its importance, process, and the valuable insights it provides to enhance the chances of a successful pregnancy.
Understanding the HSG Procedure
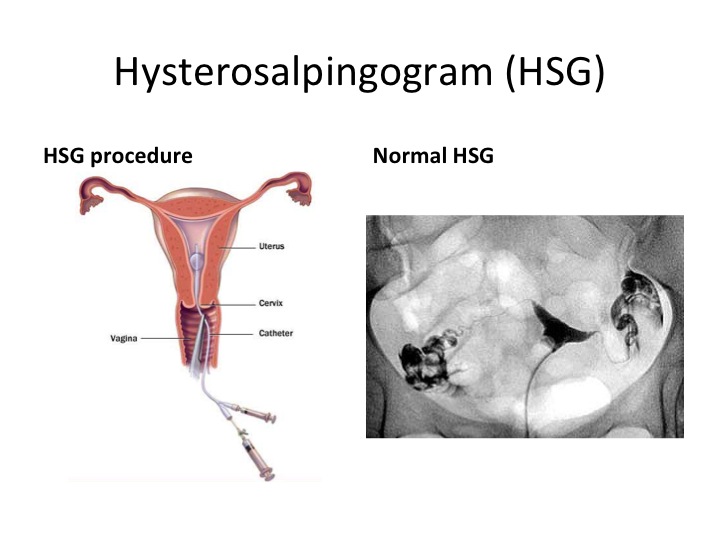
The hysterosalpingogram procedure is a specialized X-ray test that evaluates the condition of the uterus and fallopian tubes. It involves the injection of a contrast dye into the uterus through the cervix, followed by X-ray imaging to visualize the dye as it moves through the reproductive organs. This allows healthcare providers to assess the shape and structure of the uterus and detect any blockages or abnormalities in the fallopian tubes.
The Connection Between HSG and IVF
The HSG procedure plays a crucial role in the IVF process by providing essential information about the reproductive organs that can impact the success of IVF treatment. Some key connections between HSG and IVF include:
- Diagnosing Uterine Abnormalities: hysterosalpingogram can reveal uterine abnormalities such as fibroids, polyps, or structural defects that may interfere with embryo implantation during IVF. Identifying and addressing these issues before IVF can improve the chances of a successful pregnancy.
- Detecting Fallopian Tube Blockages: Blocked fallopian tubes can prevent sperm from reaching the egg or hinder the passage of the fertilized egg into the uterus, leading to infertility. Hysterosalpingogram can detect these blockages, prompting healthcare providers to consider alternative methods such as IVF to bypass the blocked tubes.
- Assessing Tubal Patency: HSG can confirm the patency of the fallopian tubes, ensuring that they are open and functioning properly. This is crucial for the success of IVF, as it allows for the natural fertilization of the egg and the passage of the embryo into the uterus.
The Role of HSG in IVF Success
The information obtained from the hysterosalpingogram procedure can significantly impact the success of IVF treatment. By identifying and addressing uterine abnormalities and fallopian tube blockages, healthcare providers can optimize the conditions for embryo implantation and development, increasing the chances of a successful pregnancy.
Preparation for the HSG Procedure
Preparation for an HSG procedure is essential and involves several key steps. Before undergoing the procedure, it is crucial to communicate with your doctor and understand the necessary preparations. Your doctor will provide you with specific instructions and guidelines to follow.
One important aspect of preparation is timing. The procedure is typically scheduled within the first week after your menstrual period. This ensures that you are not pregnant and minimizes the risk of infection.
Additionally, discussing any medications you are currently taking with your doctor is important. Some medications may need to be temporarily stopped before the procedure. Similarly, if you have any allergies or adverse reactions to contrast dye, it is essential to inform your doctor beforehand.
In preparation for an HSG procedure, it is advisable to schedule the procedure within the first week after your menstrual period, discuss any medications you are taking with your doctor, inform your doctor about any allergies or reactions to contrast dye, and come prepared with any necessary paperwork and identification.
Conclusion
The hysterosalpingogram procedure plays a vital role in the IVF journey, providing valuable insights into the condition of the uterus and fallopian tubes that can impact the success of treatment. By understanding the connection between HSG and IVF, individuals can empower themselves with the knowledge needed to make informed decisions about their fertility treatment and increase their chances of achieving a successful pregnancy.
For more information regarding the hysterosalpingogram procedure, please refer to this article by Cyprus American IVF.
For any of your fertility problems, please do not hesitate to contact us. At Fertility Solutions we pride ourselves with the excellent tailored personal care we provide to our patients for their specific needs. A team member will contact you as soon as we get your message, and construct a personal treatment plan for your fertility problems in the country of Cyprus. You can also contact our clinics directly through the links below.
Cyprus Crown IVF Contact: https://en.cypruscrownivf.com/contact
Cyprus American IVF Contact: https://www.cyprusamericanivf.com/contact-us/
Dr. Halil Ibrahim Tekin (Dr. HIT) Youtube: https://www.youtube.com/@dr.halilibrahimtekin1715
Cyprus American IVF Youtube: https://www.youtube.com/@AmerikanTupBebekMerkezi